|
But they provide a useful window into understanding the differential impact of COVID-19 by race and ethnicity.A Covid-19 vaccine record card is seen at Florida Memorial University Vaccination Site in Miami Gardens, Florida on April 14, 2021. Note that these age-adjusted rates are meant to facilitate comparisons across groups and should not be confused with actual death rates for these populations. We use the CDC race/ethnicity definitions, so the white and Black categories exclude Hispanic/Latinos, and Hispanic/Latino refers to Hispanic/Latino of any race. It is causing people of color to live sicker and die quicker, because of the color of their skin.” The data on COVID-19 provide the latest proof of this enduring fact. At the same time, race gaps in vulnerability to COVID-19 highlight the accumulated, intersecting inequities facing Americans of color (but especially Black people) in jobs, housing, education, criminal justice – and in health.Īs our former colleague Dayna Bowen Matthew, author of Just Medicine: A Cure for Racial Inequality in American Health Care, puts it: “What we politely call a ‘health disparity’ is killing people of color daily. Protests against the metronomic killing of Black people, especially at the hands of police, are taking place across the country. The issue of racial injustice has rightfully joined the pandemic at the top of the national agenda. The age-adjusted COVID-19 death rate for Black people is 3.6 times that for whites, and the age-adjusted death rate for Hispanic/Latino people is 2.5 times that for whites. But accounting for the fact that the Black and especially Hispanic/Latino populations are much younger (the bars on the right), the age-adjusted death rates show larger gaps. 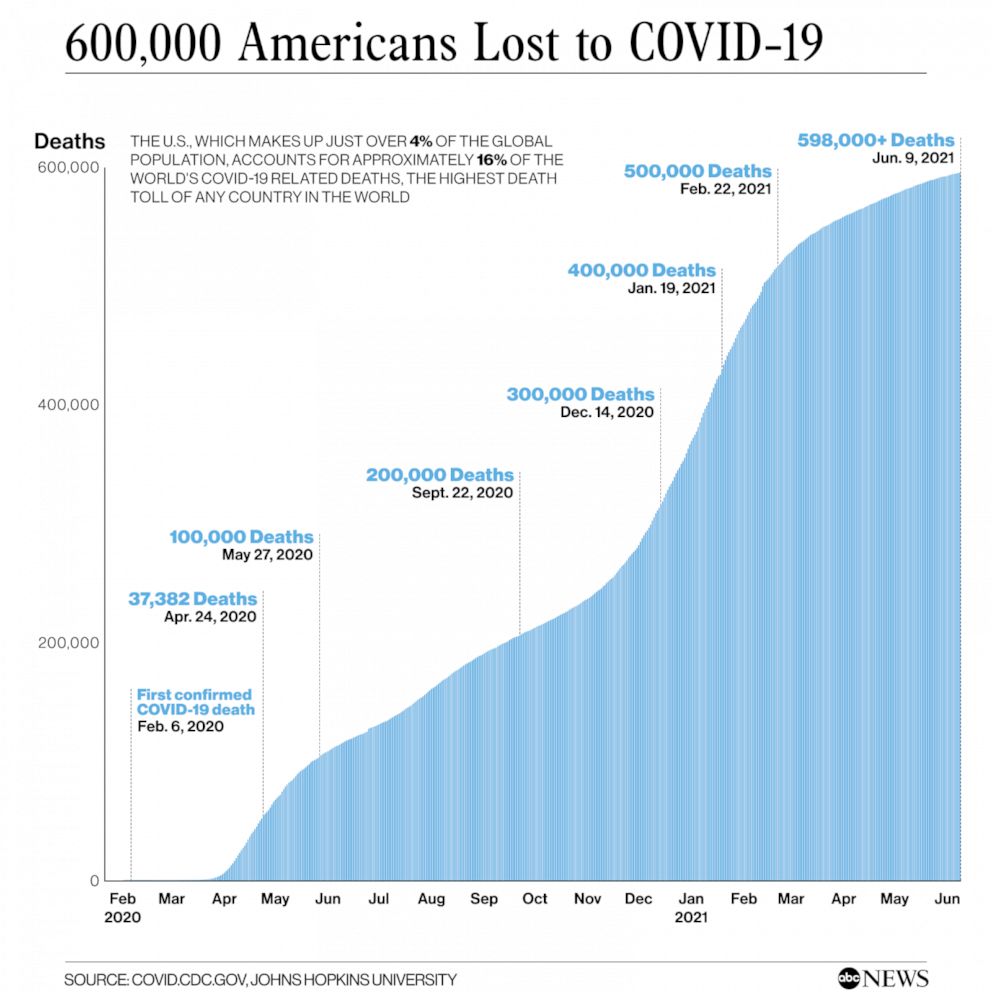
The crude death rate (the bars on the left) for Black people is twice that for whites, and the crude death rate for Hispanic/Latinos is similar to that of whites. As expected, the disparities for the age-adjusted death rates are even larger than the substantial disparities in the crude death rates: We calculate the crude COVID-19 death rates and age-adjusted COVID-19 death rates. For example, 9% of white people are over 75, compared to 4% of Black people and 3% of Hispanic/Latino people:Īge-adjusted death rates, which account for these differences in the age distributions by race, present a more accurate picture of the differential impact of COVID-19. Older people are more likely to die from COVID-19 (shown in the black line below), and whites are much more likely to be in the oldest age groups (shown in the bars), where the COVID-19 death rates are highest. It bears underlining that a much higher percentage of the white population is in older age groups. That is why we focused on age-specific death rates above. Looking harder at age and raceĪs we argued in a previous analysis on gender, the need to take age into account is paramount, given the huge age gradient in vulnerability to COVID-19. Our colleague Rashawn Ray has unpacked the structural conditions that may be causing racial inequalities in COVID-19 deaths. While geography may be part of the explanation for the race gaps, it does not look to be the main one.īlack and Hispanic/Latino people may also more vulnerable to COVID-19 if they become infected, because of less access to health care or greater prevalence of co-morbidities such as hypertension, obesity, diabetes, and lung disease – which in turn reflect broader racial inequalities. 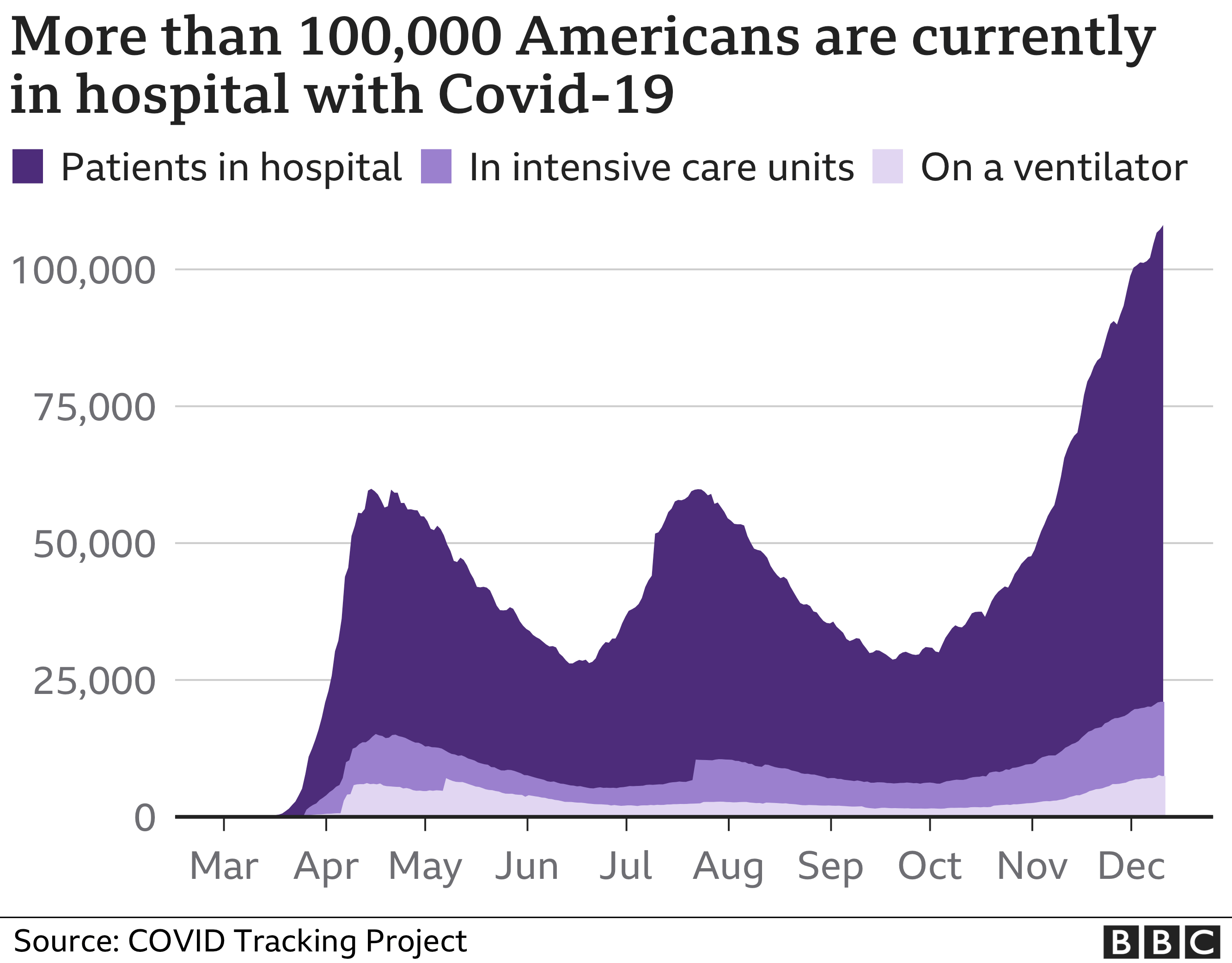
(There are concerns about data quality with regard to COVID-19 in general, including the attribution of deaths to the virus, testing rates, and so on but problems with the data are unlikely to account for these stark differences by race shown here). Critically, however, these data do not take age into account. These data suggest that Black and white people account for a slightly higher share of the COVID-19 deaths than of the population of locations where the pandemic hit hardest, while Hispanic/Latino people account for a smaller share. The CDC has produced data showing the percentage of reported deaths by race compared to the population weighted by the geography of the pandemic. The parts of the country hit hardest so far by COVID-19 have larger Black and Hispanic/Latino populations. Infection rates could be higher among Black and Hispanic/Latino people because of occupations, less social distancing – and especially geography. These factors may be influencing the risk of infection and/or the risk of death among those infected. What’s behind the race gap in Covid-19 deaths?Ī number of factors are likely contributing to the substantial race gaps in mortality rates. In that age group, 1,013 white people have died from COVID-19 (22% of the total) compared to 1,448 Black people and 1,698 Hispanic/Latino people. 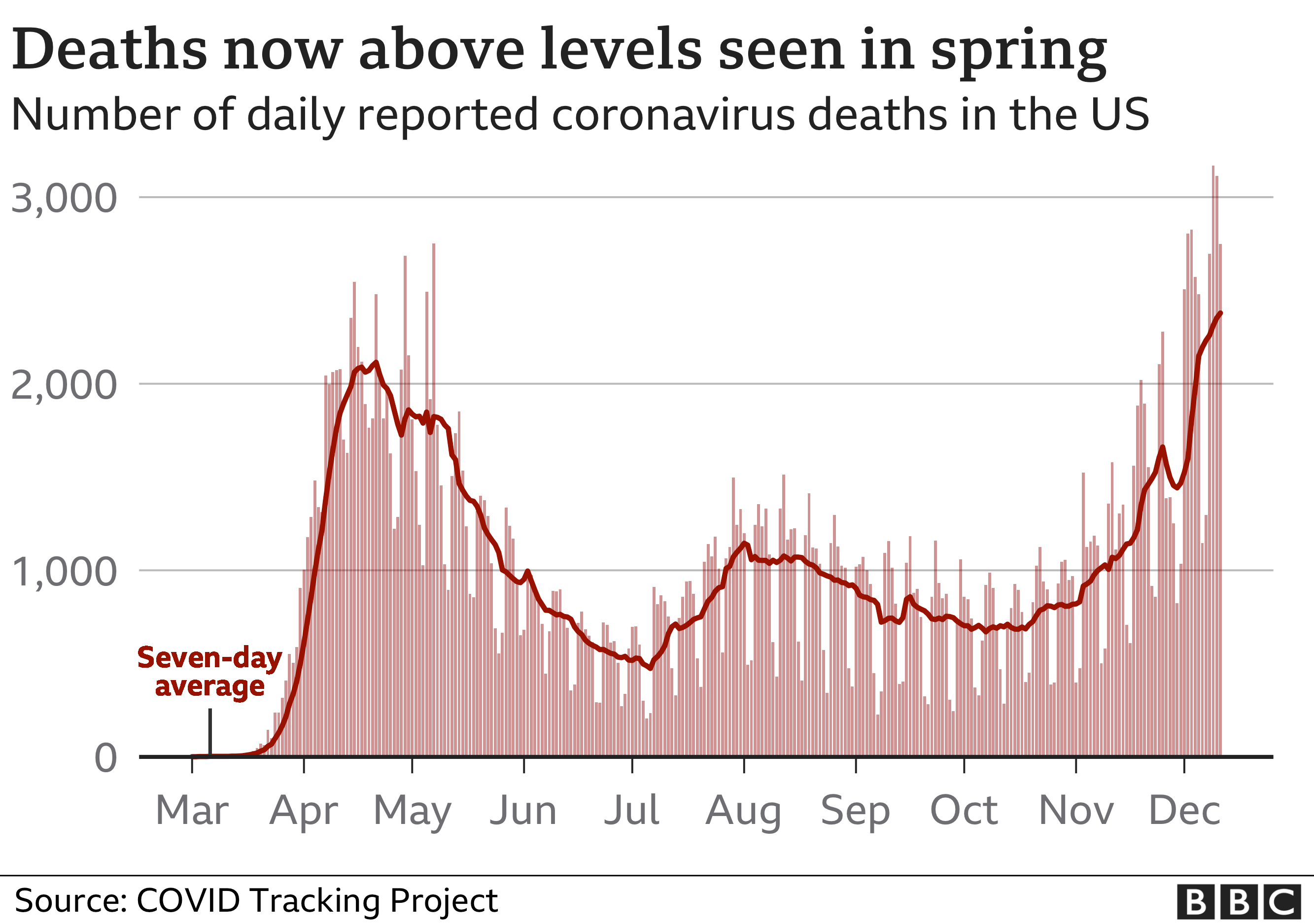
Whites comprise 62% of people in the U.S.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
